The Importance of Personal Protective Equipment for Healthcare Workers
The risk that healthcare workers endure daily has increased dramatically during the COVID-19 pandemic. According to studies performed by the Massachusetts General Hospital in the USA, “compared to the general public, frontline health care workers had an 11.6-times higher probability of testing positive [for COVID-19], and those who reported having insufficient access to PPE had a 23% higher risk.”
Therefore, personal protective equipment (PPE) serves as a barrier between infectious materials, such as viral and bacterial pollutants, and your skin, mouth, nose, and eyes when implemented properly, as directed by the Australian National Centre for Disease Control.
So, What Is Personal Protective Equipment?
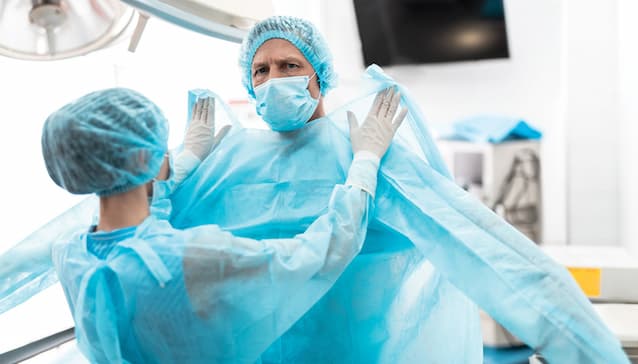
PPE is defined as “technical procedures, processes, techniques, instruments, and materials that prevent work-related injury, disease, and death.” That’s why all healthcare personnel are required to use suitable PPE when exposed to a patient with suspected or confirmed COVID-19 or other sources of SARS-CoV-2 in a healthcare setting during the pandemic.
A pair of sanitary rubber gloves, professional laboratory coat, face shields, and disposable N95 filter facepiece respirators are among the PPE available to healthcare professionals. However, variations of personal protective equipment (PPE) are needed in every workplace, not just laboratories and hospitals, because it helps prevent injuries, diseases, and fatalities. Yes, even when the world isn’t dealing with the widespread effects of a global pandemic.
Essential PPE for Health Workers
Gloves
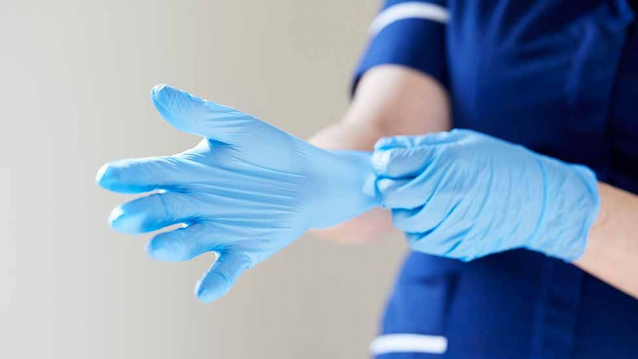
When handling contaminated equipment, or handling blood, body fluids, secretions, or excretions, gloves should be used. However, they aren’t a substitute for good hand hygiene, and they should be changed when they get contaminated, such as between patients or during procedures on the same patient. Following the removal of gloves, hands should always be decontaminated. Gloves should not be washed or reused because they are single-use equipment.
Masks
Fluid repellent surgical masks provide a barrier for splashes and droplets that could harm the wearer’s nose, mouth, or respiratory tract. They are not categorised as Respiratory Protective Equipment since they do not protect against aerosolized particles. All members of the surgical team should wear them properly, covering their nose and mouth.
If splashes of blood or body fluids are expected, a full-face visor can be used instead. They must be “CE” marked and comply with the Medical Devices Directive (MDD 93/42/EEC). Single-use items should be discarded as soon as they become soiled or after usage. Following use, they should not be kept fastened around the wearer’s neck or be reused.
Lab Coats
When working with chemicals, biomaterials, or radioactive materials, wearing a laboratory coat made from cutting-edge fabrics is essential. It’s important to remember that your protective clothing should be the right material for your research and that it should be washed regularly (NOT at home) using a GT-approved manner. In labs with open flames, 100% cotton is required.

Fit is another important element that shouldn’t be overlooked either because such coats are meant to provide an extra layer of defence for your skin and clothing. They also cover areas not covered by clothing and extend to the knees of the wearer.
Eye Protection
When there is a possibility of splashing body fluids onto mucous membranes, such as the eyes or nose, eye and face protection must be used. Goggles or a visor can be worn to protect the eyes. Personal glasses will not suffice as a substitute. If you’re using reusable eye/face protection, make sure to clean it according to the manufacturer’s instructions. After removing the equipment, thoroughly disinfect your hands.

PPE Beyond Healthcare
According to “The Best Way to Manage PPE for Employees,” here are some proactive ideas for maintaining PPE in various types of work situations, not just for healthcare workers.
Step 1: Remove any existing or potential hazards from the workplace. Management should remove a hazard that has been causing multiple injuries, such as unsafe equipment.
Step 2: Substitute a safer alternative for the hazard. If a construction worker is harmed as a result of a certain tool, the manager should replace it with safer, more effective equipment.
Step 3: Figure out a technique to finish the job without putting yourself in danger. Managers might look for options that eliminate the risk.
Step 4: Ensure that personnel have the appropriate personal protective equipment (PPE) to execute the job safely.
PPE appears in a variety of settings. Construction employees may wear helmets and work boots, whereas healthcare personnel may wear face shields and lab coats. PPE is critical in all settings because it can reduce the likelihood of employees becoming tragically wounded as a result of danger.
Having a Successful PPE Management Plan in Place
When putting a PPE plan in place, managers must consider numerous factors. First, they should ensure that all personnel are adequately taught and trained to utilise the new tools or equipment after establishing the right PPE plan for their companies or organisations. Leaders should be prepared to give their personnel technical tools and equipment.
They should also provide training and development on how to use the tools and equipment successfully. When it comes to the necessity of personal protection equipment, leaders must consider both their employees’ behavioural needs and the technical requirements of their workplaces.

Managers can help minimise job burnout and eliminate unneeded tensions for their staff on an emotional level. Employees that have a better work-life balance are more productive and have higher morale. This is in direct correlation to the minimisation of potential injuries and neglect of PPE. Managers also set an example for their employees.
They can serve as role models for how to use physical and emotional safety in the workplace. Their actions may have a detrimental impact on their employees if they aren’t correctly using equipment or have a negative attitude about using necessary tools. All of these considerations have an impact on the effectiveness of a PPE plan.



